Chronic inflammation is the world’s #1 cause of fatal disease, yet sadly it is easily prevented through living a fully optimized lifestyle.
To identify early cases of chronic inflammation and take immediate steps to eradicate it, scientists have started looking into inflammatory markers.
If there are certain biomolecules in the body that can “tell” us when chronic inflammation is taking place, we can start treating the problem a lot sooner.
Given how deadly and dangerous inflammation can be, identifying inflammatory markers as soon as possible, is a much-needed approach for practitioners focused on preventive care:
“Inflammation is a facilitating process for multiple cancer types.
It is believed to affect cancer development and progression through several etiologic pathways including increased levels of DNA adduct formation, increased angiogenesis and altered anti-apoptotic signaling.”
I’ve written several articles regarding my most recommended methods for treating inflammation.
Using testosterone optimization therapy, grounding for a few minutes a day, using supplements such as curcumin, and so on.
Today marks the first time I’ve talked in-depth about MEASURING your body’s levels of inflammation.
A Brief Overview Of Inflammation
Although inflammation is strongly linked with various cancers, it doesn’t stop there.
As I wrote in The TOT Bible:
“Cellular inflammation is the core component of many aging-related diseases. It is the chief culprit of vascular disease, erectile dysfunction, autoimmune disease, and cancer.
Low levels of testosterone have been associated with a number of chronic inflammatory diseases, including an increase in cardiovascular disease markers, mortality, diabetes, metabolic syndrome, and an increased risk for bone fracture (i.e. the bone breaking).”
But how does inflammation start, exactly?
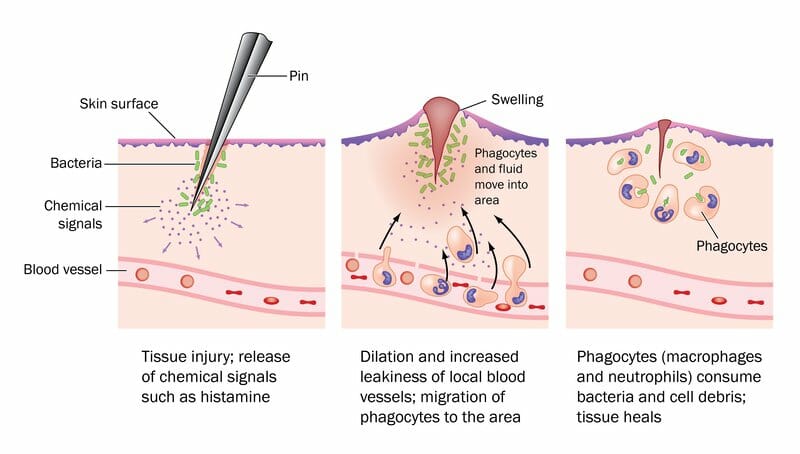
As you can see in the picture above, the body’s inflammatory response begins when one experiences a tissue injury or infection.
Following this, chemical signals are released and the immune system becomes primed to fix the damaged tissue.
The blood vessels become dilated to improve blood flow, allowing for the release of phagocytes to the injured/infected area.
These phagocytes are responsible for digesting any dying cells, debris, or dangerous particles around the site of inflammation (“swelling”).
As the surrounding cell debris and bacteria are consumed, platelets move out of the nearby capillaries to seal the wound.
This allows the tissue to heal itself and return to its original state.
Logically, one would conclude that the inflammatory response is essential for healing wounds and fighting infections.
So where does all of this go wrong?
Acute Vs. Chronic Inflammation
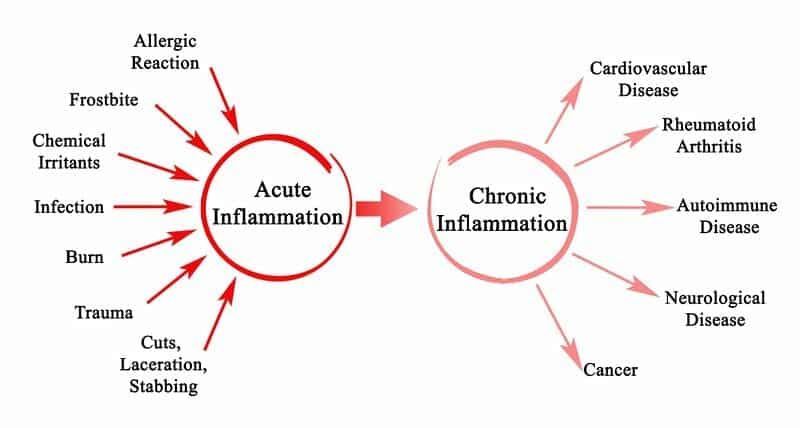
Inflammation is an essential physiologic response when it is acute (i.e. short-lived).
When your tissues are infected and/or injured, the process happens rapidly and the body returns to normal within a few days.
Chronic inflammation is what happens when the process persists for months, if not years on end.
The immune system is working overtime to treat the problem, yet does not fix what caused the injury/infection in the first place:
“Alternatively, the inflammation may stay active even after the initial threat has been eliminated.
In other cases, low-level inflammation becomes activated even when there is no apparent injury or disease.
Unchecked, the immune system prompts white blood cells to attack nearby healthy tissues and organs, setting up a chronic inflammatory process that plays a central role in some of the most challenging diseases of our time, including rheumatoid arthritis, cancer, heart disease, diabetes, asthma, and even Alzheimer’s.”
For an extended discussion on chronic inflammation and how the healthcare system has failed to treat it, I highly recommend watching this podcast I did with Dr. Roy “Buzz” Korth.
Put simply, if you treat your body poorly with a high sugar and processed foods diet, drink too much alcohol, regularly avoid lifting weights and performing cardio vascular exercise, it is a high probability your body is suffering from systemic inflammation.
In other words, you are a typical American whose biological and cellular systems are massively inflamed, ensuring you have one foot in the grave.
Want to stop being a regular American?
Keep reading.
How To Get Blood Work Done For Inflammation
Now that you understand how chronic inflammation works and why it’s imperative to treat it immediately, you need to know how to FIND it.
The absolute best way I know to treat inflammation as early as possible is through regular blood work.
Young men and women (20’s and 30’s) should get blood drawn at LEAST once a year.
Older men and women (40’s and up) should do their blood work twice a year.
You’ll want to extensively document and review all of your blood work so you can track your individual biomarkers and measure how your health is improving.
When you compare your current results to your baseline results, you’ll be able to see the changes for yourself.
And while this goes without saying, your physician should be documenting these results and openly sharing them with you.
But what precisely should you be looking for?
Based on my experience with thousands of men and women I’ve spoken with, here are the # key inflammatory markers you want to measure…
Inflammatory Marker #1: C-Reactive Protein (CRP-HS)
CRP levels rise when your body is inflamed, and is secreted by your liver as a “healing signal” for the immune system to respond to.
However, as I wrote in The TOT Bible, CRP is also very well correlated with one’s risk for heart disease.
And as it can be affected by several lifestyle factors (intense physical training, colds, etc.), your physician must take your activity into account when looking at your numbers.
Nevertheless, CRP is now commonly used to measure systemic inflammation levels.
What To Look Out For: You should be concerned when CRP is ABOVE 3.0 mg/dL.
Make sure your doctor specifically tests for “high-sensitivity CRP” (hs-CRP) as it is a far more accurate account of your body’s CRP levels.
Inflammatory Marker #2: Homocysteine
Homocysteine is an amino acid that is associated with several diseases (stroke, Alzheimer’s, etc.) when its blood levels are elevated.
In this situation, homocysteine is believed to damage arterial walls and contribute to plaque formation.
High homocysteine levels are usually the result of high body fat and excessive consumption of alcohol.
What To Look Out For: You want your homocysteine levels between 4.4 and 10.8 mmol/L for optimal health.
Anything higher than 10.8 mmol/L means you are at greater risk for cardiovascular disease.
Inflammatory Marker #3: Glycated Hemoglobin (HbA1c)
Also known as Hemoglobin A1c, HbA1c is typically used to measure your body’s blood glucose levels (and by extension, your insulin sensitivity).
Recently, it has gained attention as a potential marker of inflammation in non-diabetic patients.
What To Look Out For: Non-diabetic individuals should strive for an HbA1c reading between 4% and 5.6% (20 mmol/mol – 38 mmol/mol).
In the 5.7% to 6.4% range (39 mmol/mol – 46 mmol/mol), you have a greater chance of getting diabetes.
Truthfully over 5.7% is already pre-diabetic or well on the way to being diabetic.
And when you’re higher than 6.5% (48 mmol/mol)���congratulations, you have type 2 diabetes as your chemo-receptors in your pancreas are now non functional.
It also goes without saying that fatter people(insulin resistant) with higher levels of circulating insulin will have higher HbA1c levels.
Inflammatory Marker #4: Visceral Body Fat Levels
While this technically isn’t a blood test, this is pretty easy to measure.
If you’re fat, LOSE IT ASAP!
Not only are higher body fat levels linked to chronic inflammation, but you’re also setting yourself up for numerous estrogenic side effects (emotional mood swings, poor erectile strength, etc.).
Being fat ends up lowering your testosterone levels and diminishing your overall quality of life.
Visceral body fat is one of the most inflammatory substances inside the human body.
When it covers the internal organs (belly or gut fat), you have a high probability of contracting one of the horrible diseases of aging (cancer, heart disease, neurodegenerative disorder etc).
What To Look Out For: If your body fat is higher than 20%, you need to prioritize getting lean immediately.
You can get your body fat levels measured through a DEXA scan, or by a professional who can properly do a 7 or 11 point skin fold body fat measurement.
Aim to get your body fat down to at least 15%.
Inflammatory Marker #5: Triglycerides
Increased triglyceride levels have been linked to a number of inflammatory diseases such as rheumatoid arthritis, atherosclerosis, and psoriasis.
Elevated levels of triglycerides in the bloodstream have also been associated with vascular inflammation in diabetic patients.
What To Look Out For: According to the Cleveland Clinic, you should strive to keep your triglycerides reading lower than 150 mg/dL.
Anything between 500 mg/dL and 1,000 mg/dL increases your chances of contracting pancreatitis.
If you’re obese or diabetic, your reading could be higher than 1,000 mg/dL!
Inflammatory Marker #6: Lipoprotein-Associated Phospholipase A2 (Lp-PLA2)
While commonly known as a biomarker for cardiovascular disease, Lp-PLA2 has been shown to be a very specific indicator for vascular inflammation (rather than systemic inflammation)
Interestingly enough, its predictive ability is both independent of CRP-hs and complimentary to it for predicting one’s risk of having a stroke.
This is due to high levels of Lp-PLA2 being correlated with fatty deposits in your arteries that restrict blood flow.
What To Look Out For: The University of Rochester Medical Center states that your Lp-PLA2 levels should be lower than 200 ng/mL.
Anything higher indicates a strong likelihood of your arteries being heavily inflamed.
If both your hs-CRP and Lp-PLA2 readings are high, your risk of having a stroke will also be high.
Inflammatory Marker #7: F2-isoprostene
When free radicals in your body catalyze the oxidation of arachidonic acid, F2-isoprostanes are formed.
F2-isoprostane levels are positively correlated with increased expression of inflammatory markers such as CRP and interleukin-6.
One meta-analysis even revealed a strong link between elevated F2-isoprostane levels and diseases such as cystic fibrosis, congestive heart failure and alcoholic liver disease.
What To Look Out For: The Cleveland Heart Lab recommends keeping your F2-isoprostane levels below 0.86 ng/mg.
High F2-isoprostane levels (>0.86 ng/mg) are usually seen in people who are sedentary, eat a crappy diet and smoke cigarettes.
Inflammatory Marker #8: Myeloperoxidase (MPO)
MPO is an enzyme produced and released by white blood cells when your arterial walls are damaged.
When MPO levels are elevated, it leads to plaque formation along the walls and makes the plaque more vulnerable.
In doing so, it is responsible for the arterial walls becoming chronically inflamed (also known as atherosclerosis).
What To Look Out For: Boston Heart Diagnostics provides a “sliding scale” by which to interpret MPO readings.
- Optimal: <470 pmol/L
- Borderline: 470-539 pmol/L
- Increased Risk: ≥540 pmol/L
- Alert: >1658 pmol/L
Once you’re at “Increased Risk” and beyond, you have a greater chance of a major adverse cardiac event within the next 6 months.
Inflammatory Marker #9: Low-Density Lipoprotein (LDL) & High-Density Lipoprotein (HDL) Count
The American Heart Association does a good job of describing the difference between HDL and LDL:
“LDL cholesterol is considered the “bad” cholesterol, because it contributes to fatty buildups in arteries (atherosclerosis).
This condition narrows the arteries and increases the risk for heart attack, stroke and peripheral artery disease, or PAD.
HDL cholesterol can be thought of as the “good” cholesterol. (So, in the case of HDL cholesterol, higher levels are actually better.)
Experts believe that HDL acts as a scavenger, carrying LDL (bad) cholesterol away from the arteries and back to the liver, where the LDL is broken down and passed from the body.”
As you can already imagine, HDL possess anti-inflammatory properties while LDL possess pro-inflammatory properties.
What To Look Out For: This depends entirely on whether you are looking at HDL or LDL.
In the case of HDL, men should aim to have their levels higher than 45 mg/dL…for women, the reading should ideally be greater than 55 mg/dL.
As for LDL, MedlinePlus provides the following lab ranges:
- Optimal: <100 mg/dL
- Near Optimal: 100-129 mg/dL
- Borderline High: 130-159 mg/dL
- High: 160-189 mg/dL
- Very High: ≥190 mg/dL
Chronically elevated LDL levels leaves you at risk for plaque build-up in your arteries, restricting blood flow to your heart and brain (thereby increasing your risk of a heart attack and/or stroke).
Inflammatory Marker #10: Indicators of Fatty Liver Disease (FLD)
FLD is most common in type 2 diabetics and/or people who are obese.
As a result of living a suboptimal lifestyle, fat deposits accumulate in the liver and this lead to a wide range of problems: Inflammation, decreased insulin sensitivity, higher blood pressure, and so on.
Since symptoms of FLD are often invisible or nonexistent, blood tests are required to determine if the liver is functioning properly.
Specifically, the following three enzymes need to be tracked: Alanine aminotransferase (ALT), aspartate aminotransferase (AST), and alkaline phosphatase (ALP).
When ALT and AST are elevated, the liver is damaged.
This is because both ALT and AST are attempting to treat the injury sustained to the liver (whether acutely or chronically).
Not only are ALT and AST levels elevated for a long period of time, but the degree to which they are elevated is also significant.
For context, mild elevations are 2-3 times greater than the normal range, and severe elevations are 10-20 times greater.
ALP, while also found at very high concentrations in the liver, is responsible for breaking down proteins.
ALP levels are elevated when bile ducts are unable to transfer bile from the liver to the bowels due to blockage.
Interestingly enough, ALP levels are also higher in diseases involving excessive bone formation.
What To Look Out For: For AST levels, your reading should be anywhere between 10-40 units/liter for men and 9-23 units/liter for women.
For ALT levels, make sure you stay within the 7-55 units/liter range (readings may be higher in men).
As for ALP, the normal range is 20-140 units/liter.
Where Can I Learn More About Inflammation?
If you want a comprehensive list of supplements and medications that can help reduce chronic inflammation, read Living A Fully Optimized Life.
I also have two podcasts I’ve done which talk about inflammation and its various markers in greater detail.
This episode with Dr. Suzanne Turner details how living a pro-inflammatory lifestyle can drastically impact how you age over time.
And this mind-blowing gem with Dr. Mark Gordon shows how our “sick care” system uses a FLAWED approach to treat veterans who suffer from a wide range of inflammatory diseases.
Whether you’re a pillar of optimized health or somebody who is on the brink of collapse, get your inflammatory markers checked out ASAP.
See the right doc, get the tests booked and thank me later. 😉

 Written by Jay Campbell
Written by Jay Campbell